(This is Part 29 of Dr. Pagtakhan’s column, Medisina at Politika, on Covid-19.)
[Editor’s Note: In February 2020, CFNet started publishing Dr. Rey Pagtakhan’s column, Medisina at Politika, on COVID-19. Now on Part 29 of his running commentary, Dr. Pagtakhan’s twice monthly column has kept the Filipino community and other CFNet readers continually informed about 1) the pandemic and its impact, 2) the scientific advances on drugs and vaccines, and 3) the effectiveness of public health responses, including mass vaccination as a vital step to individual protection and development of community or herd immunity.]
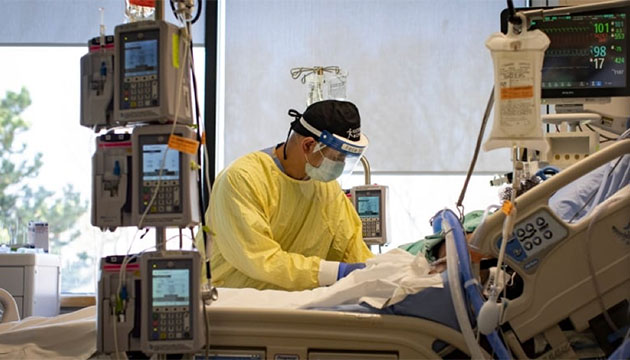
Two worst COVID-19 pandemic spots include India and the Philippines. Fortunately, Canada’s situation is not among the worst, but dire nonetheless. In Ontario where nearly two-fifths (39%) of Canadians reside, shortage of health human resources to adequately staff critical care capacity has recently become imminent. So much so that on April 16 its Deputy Minister of Health Helen Angus wrote her counterparts across the country to ascertain whom they could deploy from their departments. She identified Ontario’s specific needs: 500 nurses (ICU/Critical Care/recovery room/general), 100 respiratory therapists, 10 perfusionists, and 10 anesthesia assistants.
Ontario’s Ministry of Health has since confirmed the arrival of three medical teams from the Canadian Armed Forces and a 9-member corps of the critical care team (three doctors and six nurses) from Newfoundland and Labrador. They have come to help alleviate the pandemic crisis that has so overwhelmed the province’s hospitals and intensive care units, particularly in the Greater Toronto area, that discussion about triage had been raised, that is, doctors would be asked to make the grim choice of who gets life-saving care. These are never easy decisions to make ever.
Responses from other provinces
Alberta could not oblige. Its twin cities – Calgary and Edmonton - have seen high case numbers in recent weeks. At press time, the news reads (Heide Pearson. Global News. April 28, 2021): “Surgeries to be reduced in 3 Alberta health zones as COVID-19 cases surge.” It has also seen a recent surge of admissions of COVID-19 patients to its intensive-care units.
British Columbia remains in a precarious situation, too. Its state of emergency has once again been formally extended, this time until the middle of this month. They are under strict orders to stop travel between health regions until the end of this month’s long weekend. While no new death has occurred at press time (April 28), it reported 799 more cases.
In Manitoba, a Free Press headline reads: “No private gatherings starting Wednesday as Manitoba tries to 'dampen the third wave' (Bryce Hoye. CBC News. April 26, 2021). Most Manitobans will not be allowed to have visitors at their homes for at least four weeks. Said Premier Brian Pallister: "We're at a very critical point.” Added Dr. Brent Roussin, Manitoba’s chief public health officer: “The province is seeing rapid growth in the number of cases, hospitalizations and ICU admissions similar to what was seen in the Fall.”
“Nova Scotia just declares province-wide shutdown as COVID-19 cases surge,” reads a recent Toronto Star’s headline (Keith Doucette. Canadian Press. April 27, 2021). Premier Iain Rankin said: “COVID-19 and its variants are on the move …in every region of our province,” with a record number of new cases from its eastern, western and northern zones reported. “We need to act now,” added chief medical officer of health Dr. Robert Strang. The Royal Canadian Navy ships and Canadian Army units will deploy service personnel to assist at testing centres.
The foregoing provincial situations give a public health snapshot of the ongoing pandemic challenges Canada-wide.
The magnitude of human toll (Source: Johns Hopkins University)
Globally, the pandemic has claimed the loss of over 3.13 million lives and sickened over 148.18 million citizens. Canada’s ill-stricken population has passed the million mark (1,200,334) of whom over 24,000 had died.
Lest we forget the scope of damage on the human anatomy
![The coronavirus wreaked extensive damage (yellow) on the lungs of a 59-year-old man who died at George Washington University Hospital, as seen in a 3D model based on computerized tomograph scans. [Credit: George Washington Hospital and Surgical Theatre, 2020]](/images/photos/may2021/lungs.jpg) The coronavirus wreaked extensive damage (yellow) on the lungs of a 59-year-old man who died at George Washington University Hospital, as seen in a 3D model based on computerized tomograph scans. [Credit: George Washington Hospital and Surgical Theatre, 2020]
The coronavirus wreaked extensive damage (yellow) on the lungs of a 59-year-old man who died at George Washington University Hospital, as seen in a 3D model based on computerized tomograph scans. [Credit: George Washington Hospital and Surgical Theatre, 2020]
Reviewing the damage to the human body brought on by this disease would equip us to better appreciate its gravity beyond what statistical numbers can portray. Shown above is the three-dimensional computerized photographic scan of the lungs of a patient who died to remind all of the extensive physical damage wreaked on the human body, with these organs as ground zero. When the damaged air sacs in the lungs can no longer allow the inhaled oxygen to be exchanged for the carbon dioxide that is normally exhaled, the patients are deprived of the oxygen needed to sustain life and the elevated carbon dioxide eventually depresses the breathing center in the brain. When the heart and the kidneys fail to do their functions, the circulation stops and the toxic by-products of body metabolism accumulate. When the vascular system develops blood clots and the clots are dislodged to and block the circulation to the brain and the limbs, patients suffer a stroke and their legs, arms and toes become candidates for gangrene and amputation. And when a blood clot is dislodged to the circulation of the lungs and the brain, the consequence can be swiftly tragic.
Blot clots in almost every vital organ
Indeed, “the virus acts like no pathogen humanity has ever seen,” wrote science writers Meredith Wadman and her group a little over a year ago (Science. April 17, 2020). They were sketching the devastation the virus, since named SARSCoV-2, can inflict on the human body from head to toes among the critically ill five per cent (5%) of the patient population who died. The medical community has since learned that within the organs of those who succumbed from lung, heart and kidney failure; who died from brain stroke; and who developed multisystem inflammatory condition a month or longer after COVID-19 – as has been observed in children – is the widespread presence of blood clots.
Professor and blot clot expert Dr. Alex Spyropoulos at the Feinstein Institutes for Medical Research in New York said in a recent interview (Maggie Fox. CNN. April 20, 2021): "I have been doing this for a quarter century. I have never seen these levels of blood clots. It (COVID-19) is the most blood-clotting disease we have ever seen in our lifetimes." He observed that pathologist found blood clots in 'almost every organ' during autopsies on COVID-19 patients who died. Thus, he wondered “how ironic that fears about a much, much rarer type of blood clot (following vaccination) may now scare people off getting vaccinated when getting vaccinated against COVID-19 can prevent blot clots altogether by preventing the infection in the first place.”
Grief, helplessness, frustration, exhaustion, disbelief weigh heavily on bereaved and workers
The extensive damage is not limited to the structure and function of the patients’ human anatomy. The human loss is multiplied many times in the loved ones, families and communities left grieving and helpless. The caseloads of patients in hospitals and their intensive care units have weighed heavily on the healthcare workers – nurses, doctors and other members of the healthcare team. As they bear the burden on the front lines, burnout becomes a clear danger that could further endanger hospitals.
One recent example came from nurse Kendall Skuta at Abbotsford Regional Hospital in British Columbia. Depicted in the heart-rending photo of herself sobbing after watching a patient suddenly succumbed to the disease, she posted it to Instagram (photo below) to plead with fellow citizens to take the pandemic seriously and to heed the public health guidance.
"Please, I'm begging you all. Stay home, wear a mask and get vaccinated if you're eligible. We are all exhausted, and I don't know how much more pain my heart can take," she shared with a CBC reporter (Anita Bathe. CBC News. April 21, 2021). A plight that has been re-echoed by the president of the British Columbia Nurses' Union, Christine Sorensen, who said: "Nurses are being stretched to the limit of emotional and physical exhaustion.”
 Photo of nurse Kendall Skuta posted to Instagram after watching a patient die of COVID-19. (Credit: CBC News, April 21, 2021, with photo submitted by K. Skuta)
Photo of nurse Kendall Skuta posted to Instagram after watching a patient die of COVID-19. (Credit: CBC News, April 21, 2021, with photo submitted by K. Skuta)
In Quebec, the head of the ICU at the Jewish General Hospital Dr. Paul Warshawsky, who has attended to nearly 300 critically ill COVID-19 patients since the pandemic’s onset, confided to CBC national reporter Alison Northcott (CBC News Montreal. April 27, 2021): "We've been doing this consistently for over a year now, which is exhausting. We're hoping that the third wave is the final lift."
Additional professional pain in the midst of exhaustion and patients’ doubt
National CBC reporter Alison Northcott has captured another human dimension – the disheartening pain intensive care physicians have experienced, that is, hearing denials from their ICU patients about the role of the microbial disease in their ill health. She quoted Dr. Warshawsky saying: "We have people who have COVID who don't believe in COVID…We have to try and persuade people that we really do know what we're talking about. We've treated a lot of patients with this condition at this point."
His colleague Dr. Blair Schwartz added: “Virus skepticism can be disheartening, but his team is dedicated to getting patients through COVID's unpredictability and severity…Patients who pull through and eventually get better is what …give him hope for those stuck in the trenches of their illness, as well as for their families. That's the hope that we keep. That's what keeps the team motivated …That's the humility of being an ICU doc in COVID."
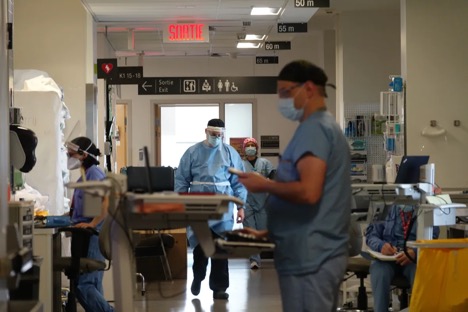 (Credit: Alison Northcott. CBC News Montreal. April 27, 2021 - Staff at the Jewish General Hospital's ICU — including Dr. Blair Schwartz, right, and Dr. Paul Warshawsky, centre — are exhausted and hope the third wave of the pandemic is the last one.)
(Credit: Alison Northcott. CBC News Montreal. April 27, 2021 - Staff at the Jewish General Hospital's ICU — including Dr. Blair Schwartz, right, and Dr. Paul Warshawsky, centre — are exhausted and hope the third wave of the pandemic is the last one.)
Toronto critical care physician Dr. Alex Patel had a similar disheartening experience. "I just admitted 3 patients to the ICU in 30 minutes. All of them had qualified for the vaccine over a month ago but never got it.” His plea to the public: “Please DON’T HESITATE when it’s your chance. It may be your last."
Status of vaccination
As of April 28th, Canada has vaccinated over 12 million (12,826,266), that is, a little over a third of its population, with 2.7% (1,018,381) fully vaccinated. The province-by-province vaccination rate all equal to about a third of each population. Nunavut has vaccinated 70% of its people; Yukon and the Northwest Territories have each vaccinated their entire population.
Dawn is coming, spark of good news
Getting vaccinated as soon as possible will protect us individually and help reach community or herd immunity. When reached, the virus could no longer spread and the pandemic ends. Heeding all public health orders and restrictions and strict adherence to public health advice – masking, keeping the distance, avoiding congregate gatherings, and washing the hands with soap and water or hand sanitizing will slow down or help halt the transmission and flatten the pandemic curve. Then, we will effectively be preventing preventable COVID-19 – disease and death. This is the ‘spark of good news’ that Canada’s Chief Public Health Officer Dr. Theresa Tam has alluded to, recently. “For the first time in many weeks, the epidemic has dropped out of a growth pattern,” she said, as a result of stronger public health measures taken the last two weeks.
The public health measures are the ones that will resolve the dire situation our health care system is in as well as help ease the emotional pains of our health care workers. When reached, then we can all celebrate our civic duty to each other. Indeed, if only the entire public would open their minds, be humble to acknowledge medical science, and heed the heartfelt voices of the healing professions – our health care team and public health officials - then we can all fulfill our sense of purpose, our collective citizenship.